As we enter into the final months of a challenging winter, fitness business owners are fighting to keep their businesses alive while simultaneously keeping their members safe from COVID-19.
As more contagious variants of SARS-CoV-2 pop up throughout the world, we are in a three-way race between vaccine roll-out, viral mutation and spread, and effectiveness of public health measures.
Inspired by Spenser Mestel’s discussion regarding best practices for gyms for controlling the pandemic, we wrote an article focused on research-based actions that gym owners can take to minimize the risk of COVID-19 transmission in their facilities.
It’s also important to note that nothing we do can fully eliminate risk and everyone should make decisions about what they do based upon their own risk tolerance. Gym owners should not be telling members that the gym is completely safe, but should instead be communicating about risk in a way that allows people to make informed decisions.
Editor’s Note: This article is not intended to be used in place of guidelines or advice from federal, state, or local authorities. This article was authored as a partnership between Todd Nief and Dr. Bryan James. Todd is the owner of South Loop Strength & Conditioning in downtown Chicago, and Bryan James is a PhD epidemiologist at Rush University who trains at Goose Island CrossFit.
Read more: The CDC’s COVID-19 Employer Information for Gyms and Fitness Centers
Superspreaders, Aerosol transmission, and asymptomatic spread
One of the most counterintuitive things about COVID-19 is that it can spread rapidly throughout a community even if the average infected individual infects less than one other person. (1)

This is caused by the dynamics of “superspreader” events, the most famous of which is a Seattle choir practice in which one individual spread COVID-19 to 53 others. (2) In this study, researchers estimated that 19% of cases seeded 80% of all transmission in 1000+ COVID-19 cases in Hong Kong last year. (3)
Superspreading events can happen in gyms, as well, like a spin studio in Hamilton, Ontario that was the source of 61 infections and an Orange Theory in Elmhurst, Illinois that was the source of 15 infections. (Note that members were not wearing masks while training in either of these situations.)
Fortunately, the standard steps to prevent COVID-19 transmission are effective in preventing superspreading events as well.
COVID-19 also presents specific challenges for fitness businesses since people can spread the disease without being symptomatic — and they can spread the disease to others who are far away without coughing or sneezing.
The standard model of spread for respiratory diseases like influenza and various common colds involves symptomatic people coughing and sneezing. These coughs and sneezes create respiratory droplets, which then infect others by being inhaled or by landing on surfaces that others touch (these infected surfaces are known as “fomites.”)
Initially, it was assumed that COVID-19 only spread through these respiratory droplets and fomites. However, a growing number of scientists are advocating for the view that “aerosols” — small droplets that hang in the air after being emitted during breathing, speaking, or coughing — are the dominant mode of transmission. The World Health Organization is a bit more conservative in their estimation of the role of aerosols in COVID-19 transmission, but states that “short-range aerosol transmission, particularly in specific indoor locations, such as crowded and inadequately ventilated spaces over a prolonged period of time with infected persons cannot be ruled out.” Sounds like plenty of gyms meet these criteria!
“Especially since we can see the end of the pandemic on the horizon, it’s crucial that we maintain fastidious COVID-19 safety protocols to keep our members safe.”
In another cruel twist, asymptomatic or presymptomatic individuals infected with COVID-19 seem to be able to infect others. (4) In other respiratory diseases, only symptomatic people are able to expel enough viral particles to infect someone else. This makes temperature checks, contact tracing, and self-isolation effective strategies necessary for pandemic control. The original SARS outbreak in 2003 was halted through these strategies, for example. (5)

For COVID-19, on the other hand, we have the potential for people to be creating viral clouds around them everywhere they go despite showing no symptoms of disease.
Think of Pigpen from Peanuts, but with invisible SARS-CoV-2 RNA in place of dirt and dust.
This makes preventing the spread of COVID-19 much more challenging, since people can put enough virus in the air around them to infect others simply through breathing and speaking—no coughing or sneezing necessary.
[Read More: The Best Home Gym Equipment, Tested and Verified by Experts]
How to Prevent the Spread of COVID-19 in Gyms
So, how do we want to think about mitigating the spread of COVID-19 in gyms?
- We want to reduce the amount of virus particles that a contagious person can breathe into the air. We can accomplish this through mask usage.
- We want to reduce the likelihood that someone else will take in enough virus particles to cause infection. We can accomplish this through mask usage, social distancing, and sanitization.
- We want to reduce the amount of virus particles in the air after they have been emitted. We can accomplish this through ventilation and air filtering.
- We want to reduce the likelihood that someone coming into the gym will be contagious. We can accomplish this through capacity restrictions and screening questions as people enter.
Wear Masks While Training
If we do have an infectious person in the gym, the best thing we can do to prevent transmission is require everyone to wear masks — even while training.
People don’t really like training with masks on. Masks (or the lack thereof) have become an identity badge in the culture war. People’s performance on conditioning workouts is impeded when they wear masks.
Still, masks are our best option for preventing spread within gyms.
By wearing a surgical mask, the number of virus particles expelled by a contagious person can be reduced by up to 74-90%. (6) Cotton masks may be more in the 50% range. (7)

Unfortunately, masks seem to be less effective at protecting the wearer—but that doesn’t mean that they are useless. The cotton masks that most people use in gyms reduced inhalation of viral particles by 20-40% in a lab simulation. (8)
Keep in mind that these effects are multiplicative.
So, imagine person A is wearing a mask that prevents 50% of the viral particles being breathed out from entering the air. Meanwhile, person B is wearing a mask that reduces the amount of viral particles breathed in by 30% (still allowing 70% through). That means person B will only breath in about 35% (50% x 70%) of the viral particles they would have otherwise been exposed to. While person B still may take in a dose of the virus, masking may reduce that viral load below the level necessary to cause a new infection.
Think about someone standing six feet away from you who starts peeing. If they’re wearing pants, that would probably make you feel a lot safer from being exposed to “pee droplets.”
Some areas have mask requirements for fitness facilities and others don’t, and, even in areas with mask requirements, compliance is mixed. If we consider the likelihood that COVID-19 can be spread through aerosol transmission in indoor spaces — especially indoor spaces where people are breathing heavily — allowing people to train without masks is a high risk.
Models show that heavy breathing likely results in a much greater output of virus particles than normal breathing, although loud talking and singing are likely to produce the most output. (9)
While masks may be uncomfortable for athletes and impede performance, coaches and gym owners should instead consider the trade-offs of not wearing masks. Superspreading events at gyms are likely to cause not just increased transmission of COVID-19 in the community, but also increased regulation and potential government shutdowns of fitness facilities.
It may be easier in the short term to skirt mask rules or to allow members to make their own choices, but the long-term health of all fitness businesses depends on getting the pandemic under control.
[Read More: Best Budget Home Gym Equipment, Start Your Home Gym with Our Picks]
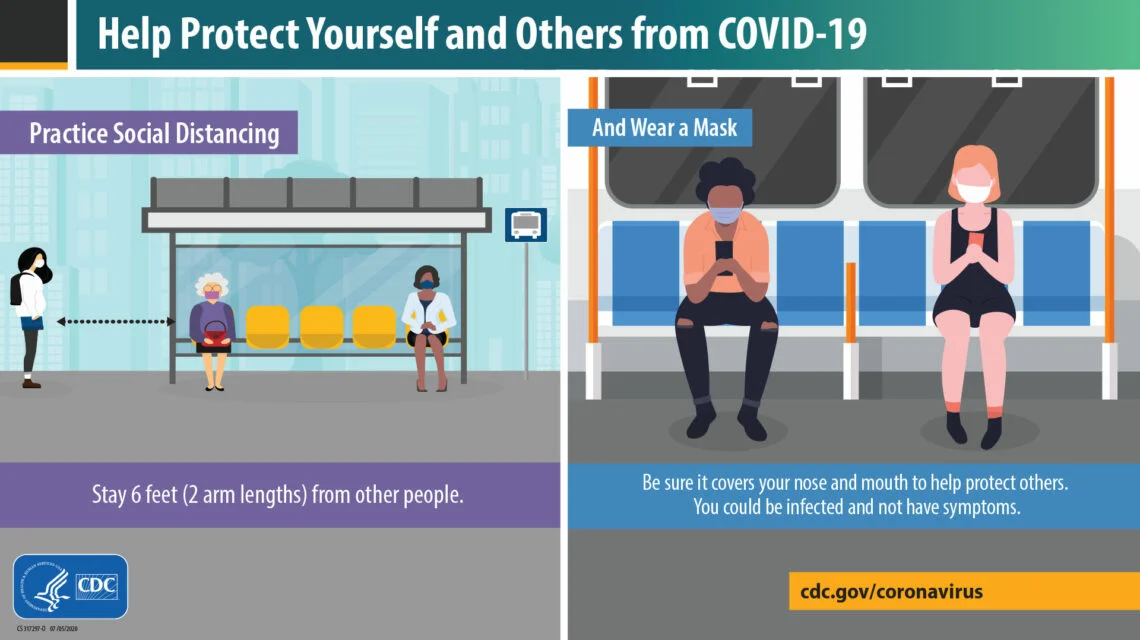
Practice Social Distancing
So now, we have small group sizes and screening protocols reducing the likelihood that an infectious person enters the gym. We have mask usage, ventilation, and air filtering reducing the amount of potential virus in the air. Even still, we may still have enough virus present to cause an infection. What can we do to further protect members?
People have been drilled with the 2m/6′ social distancing requirements for close to a year now. However, these distances may not be enough to prevent COVID-19 transmission — especially since they are based largely on respiratory droplet models of transmission rather than aerosol transmission. (10)
Still, by maintaining distance between people, we are making it less likely that someone will take in enough virus to start a new infection. In laboratory simulations of exhalation of SARS-CoV-2 virus, the viral load exposure was inversely proportional to the distance from the exhaled virus. (11) This means that keeping people further apart reduces the number of virus particles they can potentially be exposed to.
Even if we have aerosols hanging in the air, the likelihood that someone will enter someone else’s “aerosol cloud” is reduced by maintaining distance.
Wipe Down High-Contact Pieces of Equipment
At the beginning of the pandemic, people were very concerned with disinfecting surfaces — leaving their mail and packages outside packages outside for up to a week, obsessively wiping down all of their groceries, and covering their door knobs with virus-killing copper.
As we’ve learned more about the role that respiratory droplets and aerosols play in transmission, some have criticized the time, attention, and financial resources that businesses are devoting to constantly wiping everything down. The New York Times quoted Dr. Kevin P. Fennelly, a respiratory infection specialist with the United States National Institutes of Health, as saying, “In my opinion, a lot of time, energy and money is being wasted on surface disinfection and, more importantly, diverting attention and resources away from preventing airborne transmission.”
In many gyms, wiping down equipment has become a ritual enforced by coaches and the disapproving stares of fellow members. In some cases, however, wiping down equipment has taken the place of more effective measures like masking, distancing, capacity restrictions, and air filtration.
While some of this sanitization may be irrelevant and performative, wiping the surface of a treadmill, rack, weight plate or other equipment in the gym is a marginal way to reduce the likelihood of someone getting sick. When wiping surfaces, it is best to focus on areas that people are making direct contact with for extended periods of time, like barbells and dumbbell handles. And, while fomite transmission may be less of a concern with COVID-19, the increased sanitization will probably help with influenza risk. (12)
There are many options for complicated cleaning solutions and hardware. In terms of lower cost solutions, alcohol has been shown to kill the SARS-CoV-2 virus, and — despite some shortages early in the pandemic—seems to be widely available again. (13)
con
Ensure Your Gym is Well Ventilated
Even if everyone in a gym is wearing a mask, we can still have virus particles in the air inside of a gym. So, what can we do to dilute or filter this air?
If we can keep gyms ventilated so that the inside air is constantly being turned over and mixed with outside air, we can reduce the concentration of virus particles. This is best accomplished by keeping windows and garage doors open. We can also use fans to exhaust indoor air to the outdoors by setting them up pointing out in windows.
Keep in mind that we shouldn’t just be setting up fans without thinking about air flow. In fact, blindly setting up fans and internal air circulation may not be a great idea and could create more transmission risk by blowing virus particles from one person to another, as in this case of a South Korean restaurant-goer who was infected from 20 feet away based upon the airflow dynamics in the room.
In addition to increasing air turnover in indoor spaces, we also want to filter out virus particles. Fortunately, everyday HEPA filters are able to clear virus droplets.
There has been some confusion about this, since Individual viruses are small enough to pass through HEPA filters unscathed. However, the respiratory droplets and aerosols that humans expel are much larger than the individual viruses — this model found 4.7 µm to be the likely minimum size of a SARS-CoV-2 aerosol particle as compared to ~.1µm for the virion itself. (14)(15) Fortunately, HEPA filters are 99.7% effective at capturing these larger particles.
If you are looking to purchase HEPA filters for a gym, be aware that most readily available models are designed for home usage, and aren’t rated for the many thousands of square feet that most gyms occupy. Make sure to check the maximum room volume before purchasing, and recognize that you may have to purchase several filters to adequately turn over the air in larger spaces.
A more DIY-approach that could also be effective is utilizing MERV-13 filters and box fans. This is a more hacked together approach, but it is still likely to be effective as some studies have demonstrated the effectiveness of more highly-rated MERV filters in filtering viral particles. (16)
For more, here are the CDC’s recommendations for improving air circulation and filtering in buildings.
Have a Screening Process in Place
Many municipalities are introducing capacity limits for both indoor and outdoor activities. Some folks have bristled at these restrictions, claiming that they can comply with all relevant social distancing and masking requirements even with much larger groups.
While this may be true, restriction in capacity isn’t just about compliance with other protocols — it’s about reducing the likelihood that someone who is contagious is even present in the group at all.
We can think about the likelihood that someone in a group is a carrier of COVID-19 as a function of both the group size and the overall prevalence of COVID-19 in the community. This COVID-19 event risk planner from Joshua Weitz of Georgia Tech gives a rough outline of how the math works based upon a few simplifying assumptions. (17)
Using this model, the likelihood that someone in a group of a given size is infected with COVID-19 takes off shockingly rapidly as group sizes grow past 10 or 20.
Even with smaller groups, we may still have a contagious person coming to the gym. Ideally, we would be able to catch some of these folks through screening protocols.
The simplest and most commonplace method is the use of temperature checks. Temperature checks have been commonly criticized as theater, since asymptomatic and pre-symptomatic individuals can still spread COVID-19. We can improve the screening process by asking questions about symptoms or recent travel, but we will still have an imperfect process.
Still, by having some sort of upfront screening, we may be able to deter an infectious person from coming to the gym. I know plenty of people who had a headache for a few days and thought it was “probably just allergies” who ended up having a case of COVID-19. These individuals are less likely to come to a gym if they know they will have to get temperature checked and lie about a lack of symptoms in order to get their training in.
Practice Staff-Member Communication
Every gym is going to have some members who take COVID-19 more seriously than others, and others who find the requirements to be irritating and stupid.
At South Loop Strength & Conditioning, we’ve had members who seem to always find a way to toe the line of what’s acceptable with our masking and social distancing requirements in ways that maintain plausible deniability. We’ve had other members who lash out at their peers for not being diligent enough or send excoriating, multi-paragraph emails due to relatively minor protocol violations.
[Read More: The Best Budget Treadmills, Chosen By Our Experts]
This presents a huge management challenge. Coaches are left with the unenviable task of enforcing potentially dozens of constantly changing guidelines in addition to the normal responsibilities of coaching classes. On top of this, they have to manage the outsized and inappropriate emotional responses from members — some of whom are tired of being nagged about what they perceive as inconsequential violations of arbitrary rules, and others who view non-compliance as a direct threat to their health and the health of their loved ones.
All the while, gym owners are dealing with the business realities of unpaid rents, continuously dropping membership numbers, bureaucratic headaches associated with government assistance programs, and the already challenging day-to-day operations of running a gym.
As such, discussing conflict resolution with staff and even members is appropriate. Most people default to either “silence” or “violence” (and can suddenly flip from one to the other) when stressed or experiencing a conflict.
This presents as members quitting or putting memberships on hold due to lack of compliance from their peers. It also manifests as sudden outbursts or long emails when someone feels that they are being wronged or disrespected.
To get buy-in, staff can respectfully explain the consequences of not following guidelines to members: “Hey, when people see members with their masks down, we get complaints and we may even have people quit — which we really can’t afford right now.”
Staff can also create shared purpose amongst members in order to improve compliance: “I understand that you’ve already had COVID-19 and don’t think you can catch it again or spread it, but, if you don’t take the social distancing protocols seriously, it sets a bad example and puts me in a tough position. We all want the gym to be open without conflict, and having clear rules is the best way to maintain that.”
For owners, it’s important to remember that your role is not necessarily to enforce 100% compliance of all protocols, but rather to reduce the chance of COVID-19 spreading as much as possible. The “Swiss cheese model of pandemic defense” provides a useful analogy for stacking several imperfect and not always followed strategies.
While each individual strategy is flawed and has holes like a piece of Swiss cheese, sufficient strategies implemented in conjunction can significantly reduce the overall risk just as stacked pieces of Swiss cheese can present a solid barrier.
How to Communicate With Members
In 2020, SLSC had multiple members who came into the gym during the potentially contagious period of a COVID-19 infection. Many of these people were presymptomatic, and found out about their infection later when they started showing symptoms. Fortunately, it doesn’t seem like any of those members caught the disease at the gym or that they spread it within our membership.
In every case at SLSC, we engaged in a multi-tier communication strategy that seemed to work well for us.
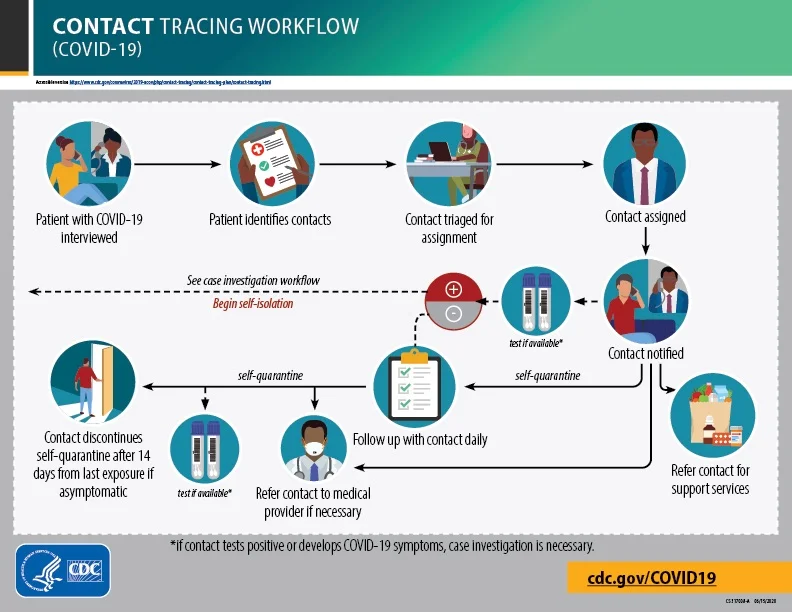
First, we immediately asked the member in question if they’d had any close contacts with other gym members or staff. Per CDC guidelines, this involves being within 6′ of someone for more than 15 non-consecutive minutes any time in the 2 days leading into either the onset of symptoms or a positive test result. With our set up in the gym, no one should be a close contact with anyone else in the gym unless they’re doing a one-on-one session.
[Read More: Best Treadmills for Walking, CPT Approved]
We did have some people who were close contacts based upon social activity outside of the gym, and we asked those close contacts to stay home from the gym and follow the CDC guidelines for self-quarantine and testing..
Then, we reached out to everyone who was in the gym at the same time as the affected individual in the five days leading into the onset of symptoms, and let them know about their potential exposure. This goes beyond the recommended two days from the CDC, but we wanted to be overly cautious and give people more information rather than less.
We did not identify the affected individual, but we did let people who asked their most recent potential exposure.
We didn’t require any of these folks who were in the gym at the same time to stay home, but we did encourage them to be extra vigilant about symptoms and to get tested if they were concerned.
We also included information about COVID testing in Chicago, and made sure to include the recommendation to wait five days after potential exposure to get tested.
After reaching out to everyone who was in the gym at the same time as the affected member, we also announced to all members that there had been a case of COVID-19 and included the total number of cases that we’ve experienced.
Our goal was complete transparency with members so that they could make risk decisions that were appropriate for them. We found that several of our members actually felt better after we’d had a few cases of COVID-19, since our communication was clear, prompt, and there didn’t seem to be transmission within the gym.
In Conclusion
Many of us in the fitness industry see a light at the end of the tunnel as vaccinations roll out across the world. Especially since we can see the end of the pandemic on the horizon, it’s crucial that we maintain fastidious COVID-19 safety protocols to keep our members safe. We don’t want to be the last superspreader event just weeks before our members would have been able to get vaccinated.
By stacking preventative measures, we can minimize the risk in our facilities, and hopefully prevent thousands of potential downstream cases of COVID-19. When thinking about interventions, we want to reduce the chances of an infected person entering the gym through capacity restrictions and screening, reduce the amount of virus they can breathe into the air through masking, reduce the viral concentration in the air as much as possible through ventilation and air filtering, and protect other members from breathing in the remaining virus through masking and social distancing.
While all of the interventions mentioned have flaws and compliance challenges, a pieced together response with less than perfect adherence will still hopefully be enough to prevent many potential infections.
Ditching the membership to build your own home gym? See our list of favorite home gym equipment to get you started.
Featured image: Damiano Buffo/Shutterstock